Tuberculosis (TB) remains one of the world’s most persistent infectious diseases, affecting millions of people every year.
While many associate TB with historical outbreaks, it continues to pose a significant public health challenge today, particularly in countries with dense populations or limited healthcare access.
Recent global events, such as the COVID-19 pandemic, have disrupted TB detection, treatment, and prevention efforts, highlighting the need for renewed awareness and action.
This article examines TB from two angles: Dr Polly Yap covers the clinical and medical aspects, explaining how the disease affects the body and how it is treated, while Dr Vivien How discusses public and environmental health, exploring how TB spreads in communities and how it can be prevented.
Understanding TB, from Symptoms to Treatment and Prevention
By Dr Polly Yap
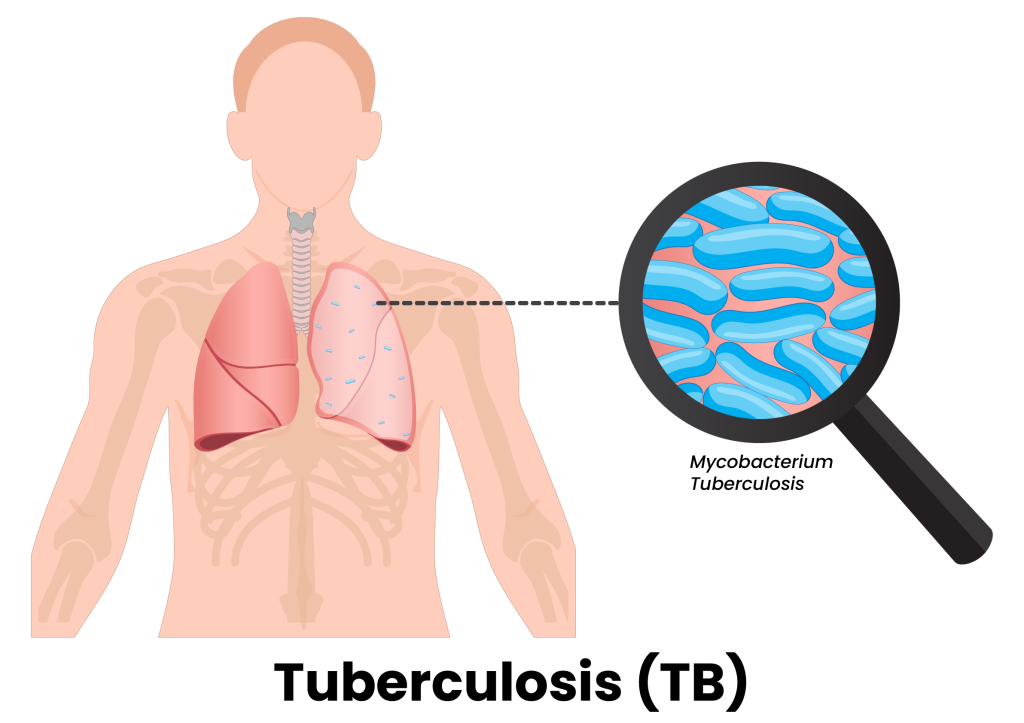
TB is an infectious disease caused by the bacterium Mycobacterium tuberculosis. While it primarily affects the lungs, TB can also spread to other parts of the body, including the brain, bones, and spine.
Recognising the Symptoms
One of the most common signs of active TB is a persistent cough that may produce mucus or even blood.
Patients may also experience chest pain, night sweats, unintentional weight loss, and prolonged fatigue. These symptoms often develop gradually, which can delay early detection if not properly recognised.
Diagnosis and Advances in Testing
In Malaysia, TB diagnosis relies on a combination of laboratory and clinical approaches. These include smear microscopy, culture tests to detect M. tuberculosis, drug, and nucleic acid amplification tests (NAATs).
Clinical tools such as chest X-rays and the Tuberculin Skin Test (TST) are also used to support diagnosis.

Advancements in diagnostic methods have further strengthened TB detection. The World Health Organization (WHO) updated its guidelines in 2021, recommending computer-aided detection (CAD) as a supportive tool for interpreting digital chest X-rays during TB screening.
Additionally, WHO-recommended molecular rapid diagnostic tests (mWRDs) have improved the accuracy of symptom-based screening, particularly among high-risk populations.
Impact of COVID-19 on TB Control
The COVID-19 pandemic significantly disrupted TB detection and treatment efforts. In Malaysia, TB case notifications dropped by about 10%, while TB-related deaths increased by 5% in 2020.
Globally, the WHO estimated that 9.9 million people developed TB in the same year. Still, only 5.8 million were able to access care, with approximately 1.5 million deaths reported.
These setbacks were largely due to delays in seeking medical care, as well as disruptions in diagnosis and treatment services, contributing to a resurgence of the disease.
Treatment and the Importance of Adherence
Treatment for TB in Malaysia typically involves first-line medications such as Streptomycin, Isoniazid, and Rifampicin, taken over a period of six to nine months.
Adherence to the full treatment regimen is critical. Even if patients begin to feel better, stopping treatment prematurely can lead to a recurrence of the infection.
Stopping treatment prematurely increases the risk of developing drug-resistant TB. It raises the likelihood of transmitting the disease to others.

Drug Resistance and Its Challenges
TB can develop resistance to medications when treatment is incomplete or improperly managed. In such cases, standard first-line drugs may no longer be effective.
To address this, healthcare providers conduct drug susceptibility testing, particularly for patients who do not respond to treatment as expected.
These patients include individuals with a history of incomplete treatment, relapse, or those from regions with high rates of drug-resistant TB.
Early detection of resistance is essential for ensuring appropriate and effective treatment.
Prevention in Everyday Life
Preventing TB begins with simple but important measures. Vaccination with the BCG vaccine remains a key preventive strategy, especially for children.
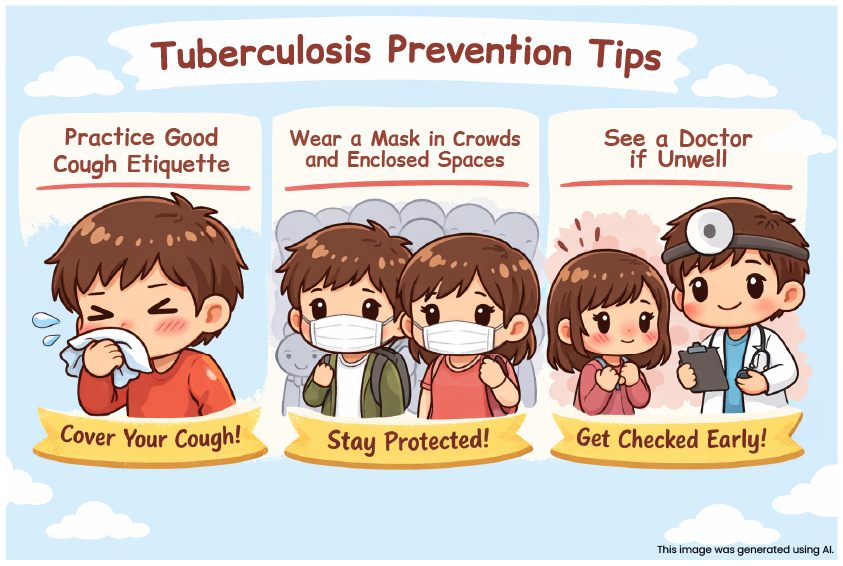
Practising good cough etiquette, wearing masks in crowded or enclosed spaces, and seeking early medical attention when symptoms persist can significantly reduce the risk of transmission.
The Role of Nutrition and Immunity
Nutrition and immune health play a crucial role in TB recovery. Undernutrition and weakened immune systems (particularly among individuals living with HIV) are associated with poorer treatment outcomes and a higher risk of early mortality.
Maintaining a balanced diet helps patients preserve body weight, strength, and energy levels throughout the long treatment process.
In turn, the body is better able to respond to medication, supporting a faster and more complete recovery.
The Air We Share: Why Tuberculosis Remains a Community Challenge
By Dr Vivien How
Imagine a microscopic traveller that remains suspended in the air long after a person has left the room. That is Mycobacterium tuberculosis.
Unlike germs that spread through touch, TB is airborne. When someone with active TB coughs, sneezes or speaks, they release tiny “droplet nuclei”.
In breezy or open spaces, these particles vanish. However, in crowded or poorly ventilated environments, like packed buses or small, shared living quarters, these invisible hitchhikers linger, spreading easily from one person to another.
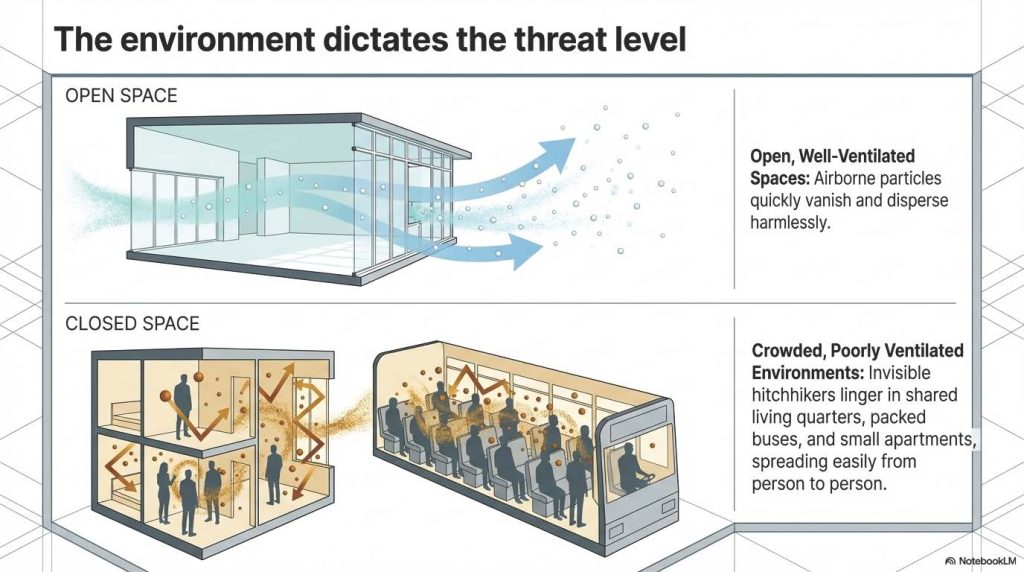
(This image was generated using NotebookLM)
The “Social Shortcuts” of TB
TB doesn’t affect everyone equally; it follows “social shortcuts” created by our modern lifestyle. Rapid urbanisation and migration often lead to dense, overcrowded housing where air stagnates, increasing exposure risks.
Global events like the COVID-19 pandemic also acted as a “curtain”, hiding TB cases. As healthcare shifted focus and people delayed seeking care, the bacteria continued to spread quietly within households and communities.
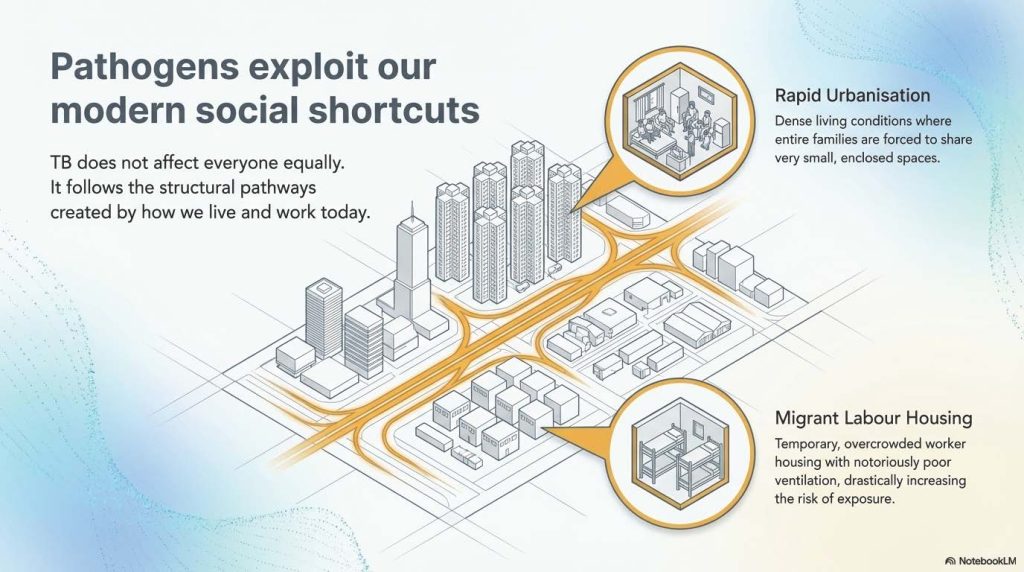
(This image was generated using NotebookLM)
Who is Most Vulnerable?
This “silent traveller” preys on those with weakened immune systems, including older people, people living with HIV, or those facing the daily stress of poverty.
Malnutrition, in particular, acts like a “broken shield”, reducing the body’s natural ability to fight infection.
In Malaysia, providing equitable care, ensuring that every person, regardless of their background, has the same opportunity to reach a full recovery, remains a significant hurdle.
The challenges lie in the “hidden costs” of care, especially the concerns of geographical disparity.
For individuals in remote areas, a single check-up can mean hours of travel and transport costs that far exceed their daily earnings.
For migrant workers, the barrier is often rooted in economic survival and fear, where the risk of losing a day’s wage or even their job security to attend a clinic appointment.
These logistical and systemic barriers often force the most vulnerable to abandon the rigorous six-month treatment course midway.
This is a challenging gap that allows the disease to persist, reminding us that our public health shield is only as strong as its reach into the most marginalised corners of our society.
Our Community Defence System
Controlling TB requires a proactive “detective” approach. In Malaysia, Active Case Finding involves healthcare teams entering high-risk communities to identify cases early.
Once detected, Contact Tracing protects those exposed to break the chain of transmission.
At the population level, BCG vaccination provides essential protection against severe forms of the disease in infants.
A Global Fight with a Local Heart
Malaysia is a key player in the WHO’s End TB Strategy, collaborating internationally to bring advanced diagnostic tools to our shores.
However, the real “superpower” is community awareness. Stigma is often deadlier than the bacteria; fear of judgment causes people to hide symptoms.
By treating TB as a curable illness rather than a secret, we help our neighbours seek help sooner.
You can be part of the solution by simply opening windows to improve ventilation and by practising respiratory hygiene.
Most importantly, remember the “two-week rule”. If you or someone you know has a cough lasting more than two weeks, seek medical attention.
While TB remains a serious public health challenge, it is CURABLE.
In Malaysia, the National TB Program ensures that testing and medication are FREE for citizens through the public health system.
By prioritising early diagnosis, we dont treat an individual; we break the chain of transmission for the entire nation.
Prepared by:
Jeffrey Cheah School of Medicine and Health Sciences
And
Associate Professor Dr Vivien How




